This is my first post and I could really use some help.
My symptoms started about 4 years ago with pulsatile tinnitus on the right and suboccipital headaches during sleep. MRA showed bilateral stenosis but no one picked it up at the time. About 2 years ago I started to have floaty dizziness, vertigo, an increase in intensity and pulsatility of tinnitus, near syncope with neck flexion. And I have this constant pulsing at the base of my skulll and upper neck. Repeat MRA identified bilateral IJV stenosis and radiologist saw it in the scan from 4 years ago.
I went to Dr. Hauser for nearly a year. Also tried chiro, myofacial release, dry needling, PT, pain management, class V laser, Graston and ART. Limited or no success. Hauser ordered CTV which again confirmed stenosis.
I consulted with Dr. Samji and Dr. Osbourne who both said they could remove the styloids but it wasn’t clear to me that this would be enough to resolve my symptoms (I think C1 may be involved). So I really dug into the research to understand it better.
At the start of this year the tide really turned. I wake up feeling exhausted, I have brain fog, memory problems, I can’t concentrate for very long, my skull is pulsing and I have a lot of pressure, on top of all the other symptoms. I’m at the ‘how am I going to go on like this’ point.
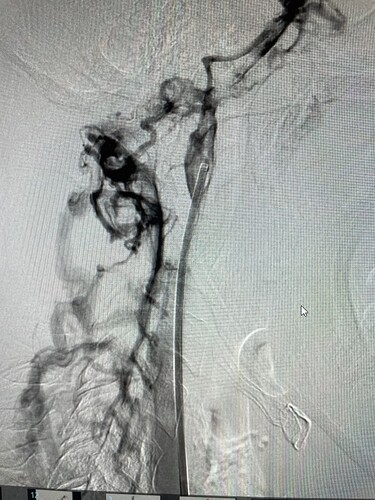
6 weeks ago I had an IR angiogram with Dr. Amans at UCSF. Again, bilateral stenosis proved. On the left there is no drainage out of the IJV supine or neck flexed, everything shunts to the right. The right is also severely blocked with everything shunting to cochlear vessels. Pressure gradient at SSS 19/0. There are significant pressure gradients throughout the venous system.
Dr. Amans said “we proved the stenosis but we haven’t proved that the stenosis is causing your symptoms”
In the meanwhile UCSF sent me to the complex neurology clinic, basically the island of misfit toys for neurological problems. This doctor was looking for what else it could be if it wasn’t from the stenosis. She thinks there could be a migraine quality to it and wants me to try Emgality.
I also had a video consult with Dr. Costantino a few weeks ago. He gave me his thumbs up for surgery but I have to wait 6 weeks to meet with Dr. Tobias. I am flying to Phoenix in a couple of weeks to meet with Dr. Nakaji. Surgery with either of them would be out-of-pocket.
Everyone I have been in contact with at UCSF, Dr. Amans, Dr. Winkler (neurosurgeon who did his fellowship with Dr. Lawton), neurologist and pain management doctor all caution against the surgery.
I am really suffering and I feel like I have tried everything in my power to try and I’m scared of the possibility that surgery could make things worse. I could really use some advice about how to proceed. I’m going to try to upload some images.
Thanks for listening to my story