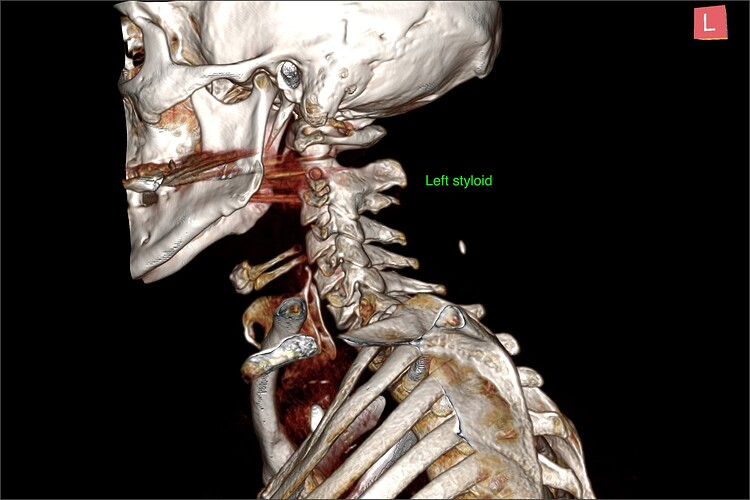
Hi all, so @Sprinter and I have been messaging and i have come up with some possible things for him to pursue in terms of further investigation. But with his permission i thought it would be useful to get some feedback, particularly from the people here who have experience reading scans @vdm @KoolDude @Chan.
Right so first lets go through the possible eagle stuff. Yes styloids are reasonably long, not huge but quick thick and pointy. They extend below C1 tubercle so therefore have possibility to impinge IJV
In axial view you can see reasonably large interval between styloid and atlas, and you can make out IJVs as this is a venogram (though not the best one i’ve seen). So i really dont think styloids are causing compression.
In sagittal view (side on), i think this is more apparent with some rounding of the IJV over the C1 tubercle.
So for the eagle stuff - i am not convinced styloids are compressing IJV but of course they could still be irritating nerves in the area.
But while studying the scans i came across something that i think is more likely causing symptoms, but could be wrong. Immediately i noticed there is quite a large scoliosis of the spine, having discussed this with @Sprinter he says he doesnt think this is coming from head position during the scan.
After a bit more looking around - his cervical spine just didnt look right which is when i noticed possibly quite an obvious malformation. His C2/3 look completely fused! Now unfortunately this does land almost exactly where the CT artefacts exist due to metal implants in the teeth - but the entire spinous process for C3 looks very small also possible suggesting congenital malformation. But the scan defects here could throw this hypothesis into doubt.
When looking from the front (and chopping part of his head off), you can see there is no disc between C2 and C3. I dont know the cause for sure, but there is a congenital malformation called Klippel Feil syndrome - causing most commonly fusion of C2/3 or C5/6. it does tend to come with a particular appearance like short neck etc. Its not something that can be acquired, but plausible he has had it asymptomatically until a head injury. Or inflammatory response/calcification etc has caused this.
There was also evidence of calcification around where the atlas meets the dens.
Looking at the sagittal view of individual slices these things are still visible.
Now looking at the MRIs you can see a similar disruption of the C2/3 disc space, its not completely calcified here but the MRI was taken many months before the CT. I also did some measurements for craniocervical instability, as my hypothesis is that the fusion of C2/3 has cause adjacent segment disease of C1/2 as is common in Klippel Feil syndrome. This would cause instability in the area, possibly evidence by the calcification around the dens.
Back to to the measurements, i’ve seen people measure the clivoaxial angle (which basically shows how the head is sitting on the neck) in different ways. Either they measure the dura (which i dont like) or they measure dens and clivus (which in my view is correct). Either way, these values should be >150 degrees, but more recent literature is saying that anything over 135 can in principle be normal. These images are very narrow however, both below 125 degrees. Possibly suggesting mechanical damage of the brainstem? But i did notice the clivus itself seems to be malformed.
On the MRI the atlantodental interval looks quite large, it isnt nearly this big on the CT but just pointing it out anyway.
Another common measurement - Grabb-Oakes line is way above the normal 9 mm cut off suggesting the cranium has translated forward over the cervical spine. Other notable things were possibly quite low lying cerebellar tonsils, suggesting a possible chiari malformation? Even in supine they do seem to extend just below the foramen magnum, so could be worse in an upright position.
Lastly the coronal (from the back) MRI view also shows a similar loss of the C2/3 disc to the CT. It also does somewhat show the head tilt and scoliosis from the CT scan also.
So to summarise, i think there could be some serious issues here. I think one of the best doctors to see in the UK about this would be Mr Jake Timothy at Leeds Nuffield to try to get a formal diagnosis, or potentially Dr Iain Smith at Newport Chiropractic.
As always - disclaimer, im not a medical doctor or radiographer and this is not in any shape a diagnosis just someone who is interested to help.